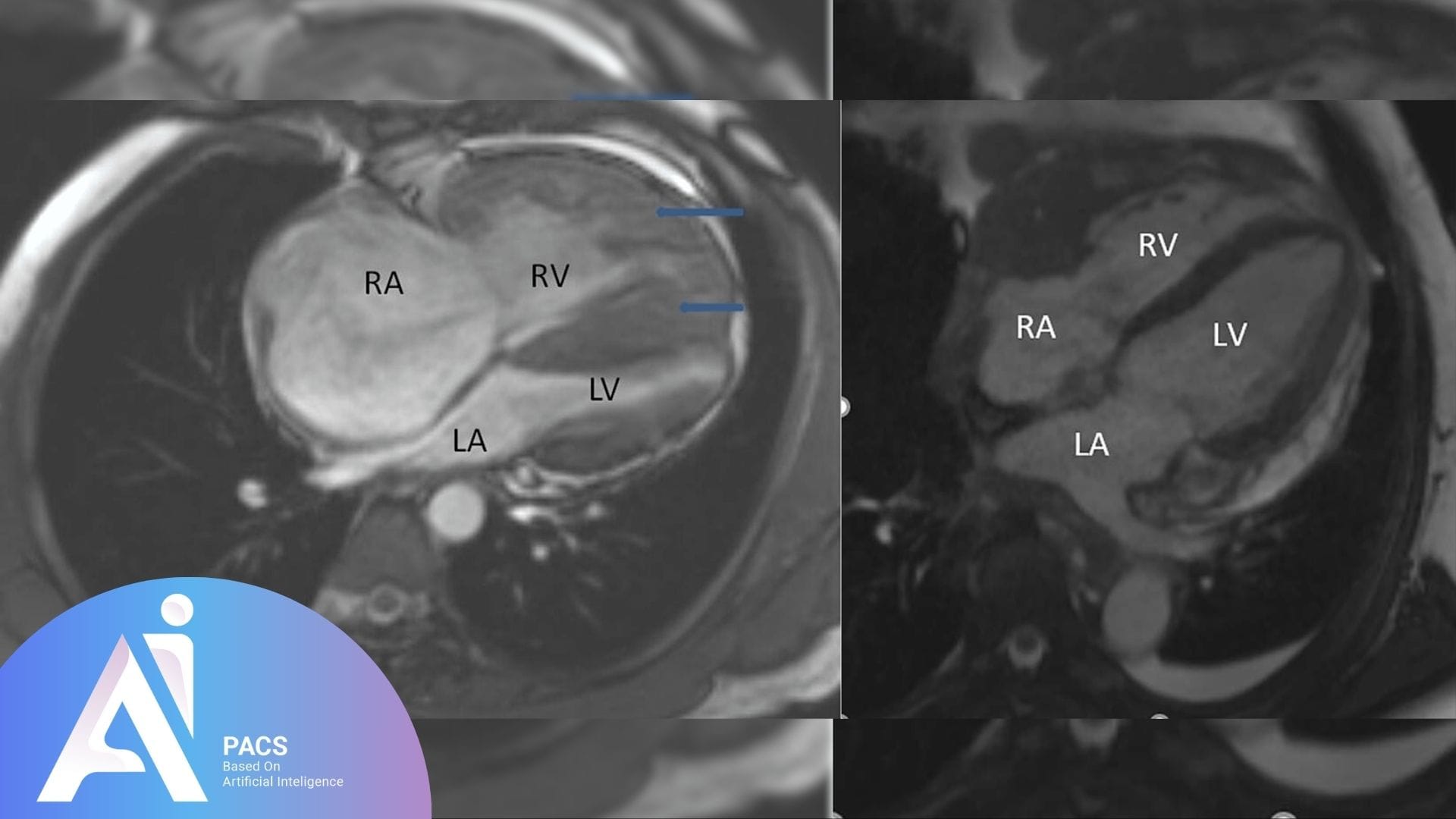
Cardiac MRI looks at the heart muscle in detail. If your report is unclear, a cardiac MRI second opinion can show whether there is inflammation, ischemia, or scar. This guide explains when the scan helps and how to use the result in your care.[1][2]
Because it combines several techniques in one sitting, it often answers the question a patient really has: what is wrong with my heart muscle, and what should I do next. The answer can guide treatment and timing. [1]
A realistic scenario
A 33‑year‑old teacher has chest pain and palpitations three weeks after a flu‑like illness. ECG is unremarkable. Echo is not conclusive. Her cardiologist orders a cardiac MRI to check for myocarditis. The scan evaluates swelling, tissue injury, and whether there is any permanent damage. A clear report helps her team decide on rest, medication, and follow‑up. [1][2]
Quick answers for Why, When, Who
Why do imaging for this problem?
• It can confirm or exclude myocarditis using tissue markers that look for swelling and injury. [1][2]
• It shows scar from ischemia and tells which muscle is still viable before procedures. [3]
• It detects infiltrative disease such as cardiac amyloidosis by measuring how the tissue space has expanded. [6]
• It does all of this without X‑ray radiation, while also measuring heart function. [1]
When should imaging be done?
• When symptoms persist yet other tests do not explain them.
• Soon after a viral illness if myocarditis is suspected. [1][2]
• After a heart attack or suspected ischemia to assess viability and guide revascularization. [3]
• When doctors suspect infiltrative or congenital heart disease and need a full map of structure and function. [4][5]
Who benefits most?
• People with red flags such as rising troponin, new arrhythmia, or chest pain that does not fit the usual pattern.
• Anyone whose treatment plan hinges on whether muscle is inflamed, scarred, or still alive. [1][3]
• Patients with known systemic conditions that can involve the heart, including amyloidosis. [6]
• Adults with congenital heart disease who need precise anatomy and function for planning care. [5]
Deeper Dive into Cardiac Imaging
How the scan sees the heart
A standard study stitches together several parts. Cine images show motion and thickening. T2‑based images look for edema. T1‑based mapping and extracellular volume (ECV) estimate tissue injury and expansion. Stress perfusion evaluates blood supply. Late gadolinium enhancement reveals scar. Put together, these pieces give a practical picture a clinician can act on. Quality relies on the right protocol, software, and experience. [1][2]
Myocarditis in plain terms
The updated Lake Louise Criteria use a simple idea. One sign from a T2‑based method for edema plus one sign from a T1‑based method for non‑ischemic injury makes the diagnosis more likely. This standardized approach increased diagnostic performance and helps avoid guesswork. [2][1]
Ischemia and myocardial viability
Late gadolinium enhancement highlights areas of irreversible injury. Segments with little or no enhancement are more likely to recover after restoring blood flow. This principle helps doctors decide who benefits from a procedure and who needs a different plan. [3]
Infiltrative disease, especially amyloidosis
Amyloid enlarges the extracellular space. Cardiac MRI can quantify this with ECV and often shows a characteristic pattern of enhancement and difficulty “nulling” the myocardium. These clues, combined with clinical data and lab tests, speed diagnosis. [6]
Congenital heart disease
In many adults with repaired or unrepaired congenital heart disease, MRI provides the road map. It clarifies chamber sizes, great vessels, shunts, and flows. This level of detail supports long‑term decisions and timely interventions. [5]
What the report means and next steps
A helpful report answers the clinical question. It should connect findings to your symptoms and history. For best clarity, share prior tests, medications, and surgeries with the interpreting doctor. Cardiac MRI is a specialized field where cardiology and radiology work together. If your report is unclear or your treatment depends on it, a second opinion is reasonable. [4]
Internal learning resources
• Understanding your MRI report
• How to prepare for an MRI scan
(Closing) Cardiac MRI offers a close look at the heart muscle. It clarifies inflammation, scar, and viability so treatment fits your situation. If you want clarity before a major decision, asking for a second opinion can help you move forward with confidence.
References
[1] ACC. Multiparametric CMR Approach to Myocarditis — Ten Points to Remember. https://www.acc.org/Latest-in-Cardiology/ten-points-to-remember/2022/07/07/19/38/Multiparametric-CMR-Approach
[2] Ferreira VM, et al. Cardiovascular Magnetic Resonance in Nonischemic Myocardial Inflammation — 2018 Update of the Lake Louise Criteria. JACC. https://www.jacc.org/doi/10.1016/j.jacc.2018.09.072
[3] Kim RJ, et al. Contrast‑Enhanced MRI to Predict Myocardial Viability and Recovery. N Engl J Med. https://www.nejm.org/doi/full/10.1056/NEJM200011163432003
[4] ACR Appropriateness Criteria — Nonischemic Myocardial Disease and related topics. https://pubmed.ncbi.nlm.nih.gov/33651982/
[5] 2018 AHA/ACC Guideline for Adults With Congenital Heart Disease. https://www.ahajournals.org/doi/10.1161/CIR.0000000000000603
[6] Kidoh M, et al. Cardiac MRI‑derived ECV and related indices for detecting cardiac amyloidosis. Radiology: Cardiothoracic Imaging. https://pmc.ncbi.nlm.nih.gov/articles/PMC10141336/
Disclaimer: This article is educational and not a substitute for personal medical care.