Understanding Breast MRI: Why, When, and Who Should Consider It in Breast Cancer Screening?
Breast MRI is a powerful and increasingly used imaging technique in breast cancer evaluation and screening. It provides high sensitivity for detecting breast malignancies, particularly in high-risk individuals or when other imaging modalities are inconclusive.
However, because MRI can also detect many benign or normal findings that mimic cancer, it carries a higher false-positive rate than mammography or ultrasound. That’s why patient selection, timing, and interpretation by experienced radiologists are essential.
A Patient’s Journey:
One Suspicious Finding and a Complicated Follow-Up: A 45-year-old woman with dense breast tissue and a family history of breast cancer underwent routine mammography and ultrasound. Both showed no abnormalities, but due to her elevated risk, her physician recommended a breast MRI. The MRI revealed a small, enhancing area that was not visible on either the mammogram or ultrasound. Because traditional biopsy methods could not target it, she needed an MRI-guided biopsy. She asked, “Why can’t we just follow this up with another ultrasound?” We explained that since the lesion was only visible on MRI, only MRI could guide the biopsy and future follow-up. The final result is benign fibrocystic change (a stressful process), but a clear answer, thanks to the precision of MRI.
👉 Upload Your Breast MRI for Expert Review
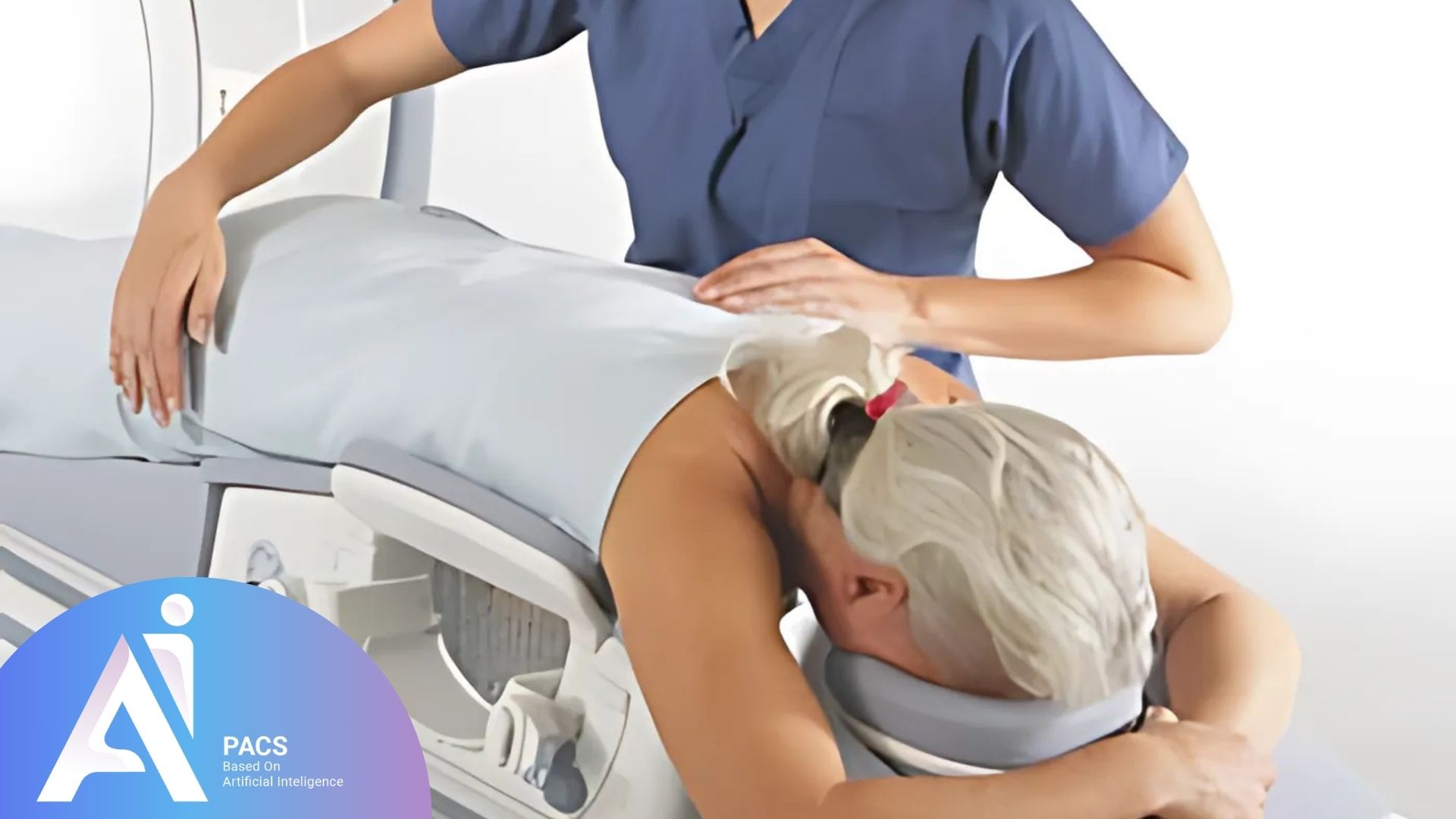
Why Is Breast MRI Important in Cancer Screening?
High Sensitivity, but Also Complexity
Breast MRI can detect cancers that mammography or ultrasound may miss—especially in:
- Dense breast tissue
- High-risk women (e.g., BRCA mutation carriers)
- Post-surgical or post-treatment evaluation
- Inconclusive mammography/ultrasound results
However, its low specificity means it also detects many benign or unclear findings. Therefore:
- A negative MRI is very reassuring
- A positive MRI often requires careful follow-up and correlation with other imaging
Role in Different Clinical Settings:
- Screening in high-risk patients
- Staging known breast cancers (extent of disease)
- Problem-solving when mammogram or ultrasound findings are unclear
- Assessing implant integrity
When Should Breast MRI Be Performed?
Key Indications Include:
- High-risk screening (e.g., BRCA carriers, strong family history)
- New cancer diagnosis to assess size or multifocal disease
- Pre-operative planning
- Post-treatment follow-up or when recurrence is suspected
- Dense breasts with equivocal findings on other modalities
MRI Screening Protocols:
Some countries now utilize abbreviated breast MRI protocols as cost-effective screening tools, particularly in resource-limited settings or to enhance accessibility. These protocols may vary in:
- Sequence length and detail
- Use of contrast
- Follow-up guidelines based on national protocols and healthcare budgets
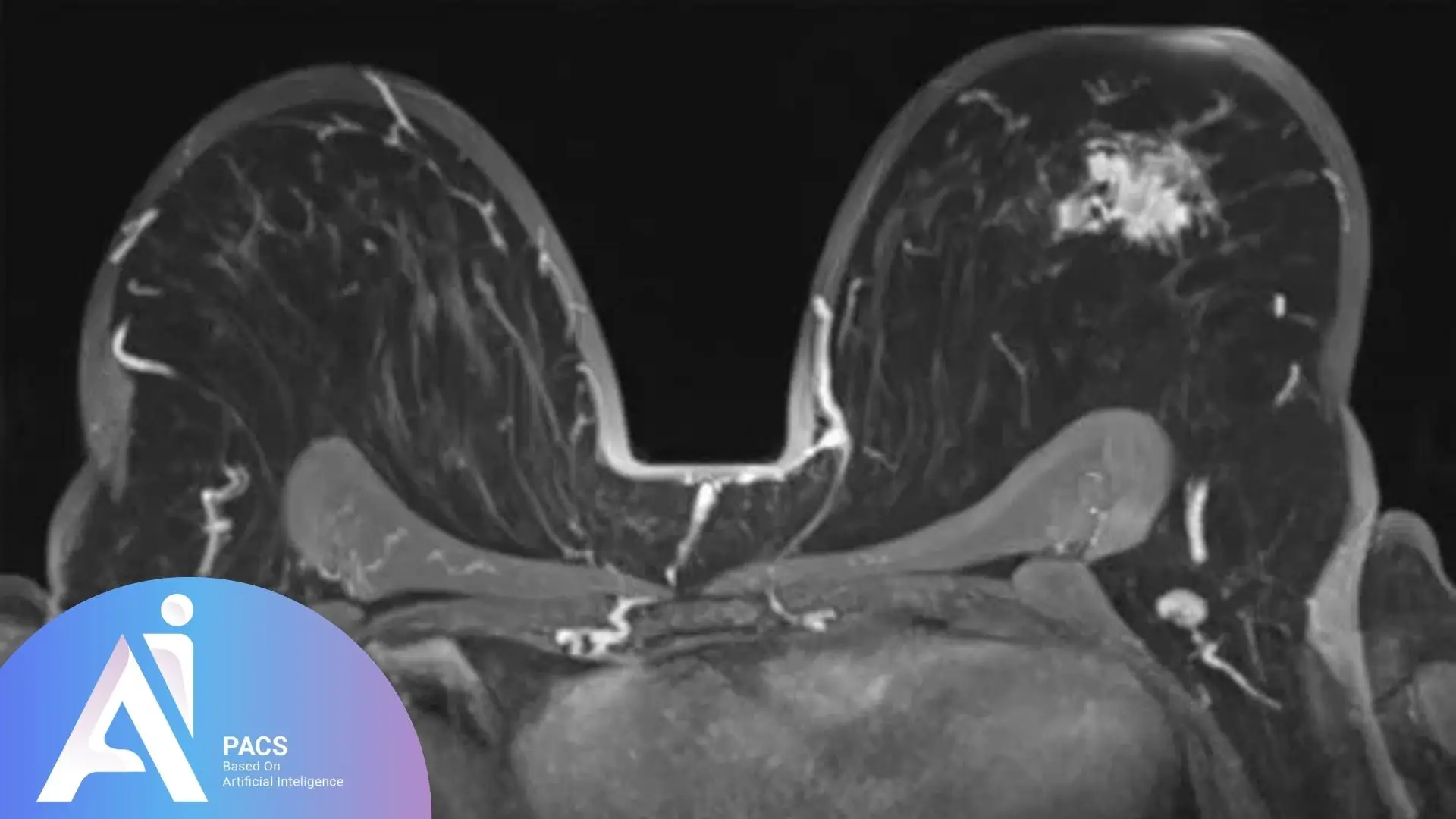
Who Should Get a Breast MRI?
Patient Categories That Benefit Most:
- Women with BRCA1/BRCA2 or other gene mutations
- Personal history of breast cancer
- First-degree relative with early-onset breast cancer
- Women with very dense breasts
- Cases where surgery or therapy decisions depend on lesion extent
Limitations and Considerations:
- MRI-guided biopsies are technically complex and not widely available
- Positive MRI without correlation on ultrasound or mammography requires MRI-only follow-up
- Results must be interpreted in clinical and imaging context
AI-PACS Is With You, Providing Expert Imaging Review
Breast MRI interpretation requires skill, context, and comparison with mammography and ultrasound. At AI-PACS.com, we offer second opinions and consultation for:
- Screening breast MRI in high-risk patients
- Problem-solving scans with unclear findings
- MRI-guided biopsy planning
Our radiologists understand how to strike a balance between sensitivity and clinical relevance.
Get your breast MRI reviewed here on our online radiology report services and take the first step towards understanding your health better.
Deeper Dive Into Breast MRI in Screening (clear, not overly technical)
Where MRI shines
Contrast‑enhanced breast MRI sees cancer‑related blood flow patterns and can detect additional, otherwise occult disease. In high‑risk patients, MRI is recommended alongside mammography; in average‑risk patients it is not routine. [1][2]
Limits and false positives
MRI’s sensitivity comes with trade‑offs: it often flags benign findings that still require follow‑up or biopsy. A negative MRI is reassuring; a positive MRI needs careful correlation and, at times, targeted biopsy. MRI complements rather than replaces mammography. [1]
Dense breasts: what guidelines say
Dense tissue both increases cancer risk and can mask tumors on mammograms. The U.S. Preventive Services Task Force found insufficient evidence to recommend for or against routine supplemental MRI for dense breasts alone, so decisions should be individualized. European guidance from EUSOBI, influenced by the DENSE trial, supports offering screening MRI to women 50–70 with extremely dense breasts, typically every 2–4 years. [3][4][2]
Abbreviated MRI (fast MRI)
Abbreviated protocols shorten scan and reading time. In the EA1141 trial, abbreviated MRI detected more cancers than digital breast tomosynthesis in women with dense breasts, though programs and coverage vary. Ask your center whether an abbreviated option is appropriate in your case. [5][2]
Timing, contrast, and safety
For cancer detection, MRI uses gadolinium contrast; non‑contrast MRI is reserved mainly for implant rupture evaluation. Most people tolerate contrast well. If you have significant kidney disease or are pregnant, your team will weigh risks and benefits and may adapt the plan. [6]
MRI‑guided biopsy and follow‑up
If a lesion appears only on MRI, MRI guidance is required for accurate biopsy and for future comparisons. Not every finding needs biopsy; your radiologist will use BI‑RADS assessment to recommend biopsy, targeted ultrasound, short‑interval follow‑up, or routine screening. [6][2]
What the Report Means & Next steps
Your report should explain the finding, BI‑RADS category, and a clear recommendation. Bring these questions to your clinician: Does this change my surgery or therapy plan? If the finding is probably benign, when is the follow‑up MRI due? If MRI shows more disease than mammography, how will that affect treatment choices? [2]
Final Thoughts
Breast MRI Is a Powerful Tool – With a Learning Curve, It Can Detect Cancer Earlier and More Clearly in High-Risk Patients. However, it requires experienced interpretation, careful follow-up, and the ability to correlate findings across multiple imaging types. This is why we’re here: to provide you with the information and expertise you need.
Whether you’re considering MRI for screening or already have results that raise questions, AI-PACS can help you find clarity and peace of mind with expert imaging review.
References
- American Cancer Society. Screening recommendations, including annual MRI for high‑risk and limits for average‑risk. https://www.cancer.org/cancer/types/breast-cancer/screening-tests-and-early-detection/american-cancer-society-recommendations-for-the-early-detection-of-breast-cancer.html
- ACR Appropriateness Criteria: Female Breast Cancer Screening. https://acsearch.acr.org/docs/70910/narrative/
- Breast Cancer Screening, Final Recommendation (2024). https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/breast-cancer-screening
- EUSOBI Recommendation: Offer MRI screening to women with extremely dense breasts. https://www.eusobi.org/news/eusobi-recommendation-breast-cancer-screening-women-with-extremely-dense-breasts/
- Comstock CE et al. Abbreviated MRI vs DBT in dense breasts (EA1141). JAMA. 2020. https://jamanetwork.com/journals/jama/fullarticle/2761645
- RSNA/ACR RadiologyInfo.org. Breast MRI patient page, including contrast use and MRI‑guided biopsy. https://www.radiologyinfo.org/en/info/breastmr
Disclaimer: This article is educational and not a substitute for medical care.